by, Lisa-Marie Sasaki Cook, BSN, RNC-OB, C-EFM, ICCE, CD
In the potentially fatal event below, a cord blood infusion really put into practice everything we already know about delaying cord blood clamping – the increased provision to the neonate of oxygen, red blood cells, stem cells, immune cells, iron reserves, and blood volume.
It was wonderful was seeing this baby go home with no apparent sequellae after a complete abruption at birth.
The mom was 17 years old and 27+5 weeks gestation when she arrived at our hospital for GBS bacteriuria, lower back pain and abdominal cramping. She stayed on our antepartum unit for five days due to cervical dilation 1-2 cm and received antibiotics and Betamethasone.
On day six, the mom complained of contractions around 0800. The resident checked her, she was 5 cm/80% and uncomfortable. We started her on Magnesium for neuroprotection, as ACOG recommends. We started her on a Magnesium Sulfate 6 gram loading dose and continued the Magnesium at 2 grams/hr.
At 1600 she was found to be 7 cm dilated and requesting an epidural. Four hours later, as she began to push, the baby began having prolonged decelerations. She brought the baby down quickly while experiencing tachysystole. With the last few contractions, the fetal heart rate plummeted as she pushed out her 1120 gm infant along with an abrupted placenta.
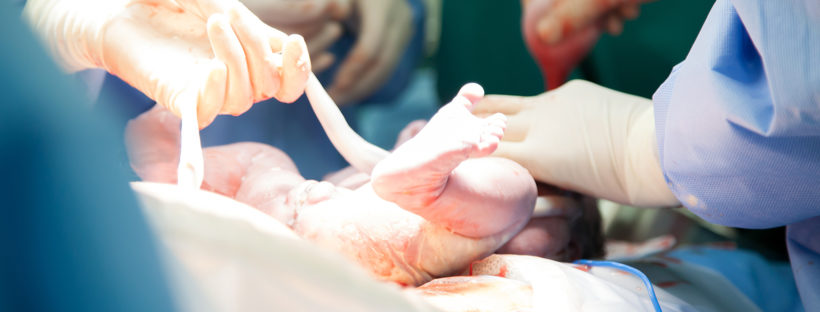
The baby’s pale, lifeless body was received by the NICU team. The physician carried both the baby and placenta to the warmer. For seven minutes, the pulsating placenta infused blood into the baby while the NICU team began to resuscitate the baby. Within the first minute, the baby gasped and cried while we watched in awe as this hypovolemic baby began to cry and turn pink as the doctor continued to hold the placenta above the baby. Baby’s APGAR scores were 7 at one minute and 8 at five minutes. CPAP and Neopuff was all the NICU team used to stabilize this neonate. Baby’s initial CBC: 10.1>15.8/46.3<272
Had we done what was “usual” and clamped the cord, would there have been enough blood cells for a successful resuscitation?
The time that it would’ve taken for them to crossmatch a sample then give adult blood with no stem cells would have been enough time for hypoxemia to occur. The baby received no blood transfusions during her hospital course of care and went home after about seven weeks of care.
Studies have also shown a reduction in newborn anemia; need for transfusion, intraventricular hemorrhage and necrotizing entercolitis. Other studies have found an increased risk for polycythemia and jaundice. In the event that hypovolemia be suspect, a cord blood infusion would be preferred and beneficial with the later treatments for possible polycythemia and jaundice provided if necessary. Based on new data and the current literature that profoundly encourages a delay in cord blood clamping, in the rare instance of a complete placental abruption this event could be modeled to save an infant’s life. This really impacted our hospital and we have since been able to do this in another case. My hope is that you’ll be able to glean wisdom from our experience.
 Lisa-Marie Cook is a Labor and Delivery Nursing Preceptor in Washington, DC and teaches AWHONN Intermediate Fetal Monitoring. She is also the CEO of Birthing Basics, LLC where she teaches evidence-based birthing classes.
Lisa-Marie Cook is a Labor and Delivery Nursing Preceptor in Washington, DC and teaches AWHONN Intermediate Fetal Monitoring. She is also the CEO of Birthing Basics, LLC where she teaches evidence-based birthing classes.
Resources
“Perspectives on Implementing Delayed Cord Clamping,” Nursing for Women’s Health, 19(2), 164–176.
ACOG Committee Opinion Number 543 (2012) Timing of Umbilical Cord Clamping.
Hutton, E.K., Hassan, E.S. (2007). “Late vs early clamping of the umbilical cord in full-term neonates: systematic review and meta-analysis of controlled trials”. Journal of the American Medical Association, 297(11): 1241-52.
McDonald, S.J. et al. (2013) Effect of timing of umbilical cord clamping of term infants on mother and baby outcomes. Cochrane Database Systematic Review, July 11. McDonald, S.J. et al. (2013) Effect of timing of umbilical cord clamping of term infants on mother and baby outcomes. Cochrane Database Systematic Review, July 11.
Rabe, H. et all. (2012) Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Cochrane Database Systematic Review, Aug 15.

Wow!
Thats a wonderful example of delayed cord clamping and the blood in the cord and placenta giving baby the blood that was needed! I’m wondering though why this hospital ( maybe it’s a small community hospital) needs to cross match for the baby- that wastes precious time! At Legacy in Portland we just call for stat Oneg blood with the moms medical record number. This has been in place now for nearly 10 years and this policy is spreading to other hospitals. Please spread the word about having blood immediately ready in case of OB emergency.
I just reread it and they had a NICU so they must be a high risk unit… Just wondering again why blood was not routinely available stat at their hospital?
Moving this example of delayed clamping into the OR could sure make a tremendous improvement in outcomes in smaller hospitals who don’t have much in the way of a blood bank though. I think this is a terrific use of baby’s own blood supply!
At Last! I have been teaching this practice for 20years. Denying any baby its full placental transfusion is a ghastly thing to do and these even more vulnerable babies require all the help they can get. Keeping them on their mother’s body will improve outcomes even more. A lotus birth where the placenta is left to come away at the navel naturally will see a further improvement for these babies. There is so much happening in front of people that has been ignored for decades that it is time to stop and reconsider many routine practices that are actually harmful to the new born.
Well there you have, Mother Nature knows best, this is obviously the way God planned it!
Fantastic. This is one for the books, literally. A tremendously smart solution. Thank you for sharing.
Beautiful.
Just wondering if this would have worked on my son when he was born! April 2, 2003, I was at 27weeks gestation and had a great pregnancy. That day I started having abdominal pain in my stomach pouch. This pain was up higher than my abdomen. I had a Roun-Y Gastric Bypass December 2000. That’s how I knew it was in the pouch. I had these pains before but would always go away. That day they didn’t. I was brought to the local hospital that I worked at by my neighbor. My husband wasn’t home at the time, he had to meet me there. First of all, my other neighbor just so happened to call and check up on me. I told her what was happening, that I was on the floor rocking back and forth crying in pain. She called the local hospital that I worked at and they said that they wouldn’t take me because it wasn’t my primary hospital. She then called my primary hospital and told them what was going on and they called the other hospital and I guess they demanded they take me. They were sister hospitals. I didn’t think I could make it to my primary due to the tremendous pain I was in. When my other neighbor was driving me that’s when I pretty much blacked out I guess. I only remember a few details like vomiting up black stuff and ripping my clothes of when I got to my room from being hot I guess. They were feeding me pain meds, morphine was one of them and GI cocktails. This all was in the evening. The internal medicine doctor ordered an US in the morning and wasn’t done until around 10am. He then consulted a surgeon. When that surgeon seen the US results he immediately called my Gastric Bypass doctor that did my surgery. He was also a general surgeon. He said to transfer me STAT. I was diagnosed with Intussuseption and was going septic. So all this time that I laid in that hospital because that IM doc never ordered anything STAT, my body was shutting down and going septic. The order was written at 5pm on April 3 and I didn’t get transferred until 11pm. I guess all the ambulances were busy that night due to an ice storm. When I finally arrived I guess I went straight to ICU as they prepared the OR room for my emergency surgery. All this time, I believe my baby was still doing fine. Although there is one section in my records that looks like they didn’t monitor my baby or that nurse forgot to write it down.My surgeon performed an emergency bowel resection at 3am on April 4 and took a foot of my bowel out. I also ended up with pancreatitis, a collapsed left lung, and ascites. I had two red robinson drains coming out of me to drain the pancreatic fluid and a feeding tube put in later because the fluid was eating a hole in my pouch because when I was trying to eat even though I was on TPN, my food was coming out of my red robinson drains. When I was in recovery they had a helicopter on stand by so that when I was done recovering they were going to fly me to a children’s hospital so that if I did go into labor they would have a NICU which the hospital that I was currently at didn’t have one. Well, while I was in recovery I went into labor. So I went back to the OR for emergency C-Section. They said they did all they could to save the baby. They then gave my son to my husband. He said our son took two breaths then died. So, I’m wondering if this procedure would have saved my son? Probably not though. He was septic because I was septic. I don’t know what all they did to try and save him. My family almost lost me to. I was in the hospital due to all the complications that I had. After I finally got out of the hospital I went to see the pediatrician that worked on my son. I wanted to know what really was the cause of my son’s death. The death certificate said Hypoxia. I didn’t get a straight answer out of the pediatrician. Was it Hypoxia? Sepsis? I know it wasn’t a still born, so I guess it was considered a newborn death? My son was 2# 14oz. and 14″ long. He would have had red hair like me from what I can tell from the pictures. I still to this day get angry at myself because I wish I would have told my neighbor to take me to my primary hospital. I should have known better to go to a small town hospital, but I didn’t think I could handle the pain driving that far away. It was a 35min drive. I thought that because I was an employee at that first hospital that I went to, I would have been treated better and faster. I should have had my parents drive me instead of waiting on that ambulance. I don’t remember hardly anything that happened. I was so drugged up because I was so sick that I don’t remember. I don’t remember having my son’s bassinet next to me in the ICU. Or me holding him or his features. I don’t even remember holding him a couple days later when they took him out of the morgue for my inlaws to be able to see him. We had him in the morgue because they had to fly in from out of state. I vaguely remember any of it from the day I first went in to the day I got released which was a month later. All I have are pictures of him to look at, not the memory of holding him or seeing in with my own eyes. That’s why I get so angry!!! Anyway, I know you all didn’t need to hear that story, but I figured if I only gave minor details, that someone would ask me questions to go into more detail.
Dear Melissa, I don’t have any answers for you about the birth or loss of your son, but I just wanted to send my condolences and a strong, long hug. Your story brought me to tears. I am so sorry that you went through such pain and trauma, and I can only imagine the magnitude of emotions you must continue to feel, especially since your memories are blurred and strained. It makes sense that finding a sense of closure and peace with what has happened would be incredibly difficult for anyone, but maybe even more so without having clear answers or memories. I am so sorry and my heart goes out to you and your family. I hope you are able to find some peace. Your angel baby sounds like a beautiful little soul, even if his time earth side was brief. Love and light!
What a wonderful story of a great rescue and sharp thinking by the OB team! Please keep sharing stories like these so that we can all learn from your experiences!
One small edit. Placentas can not pump….but the baby’s heart was still pumping blood to the placenta in an attempt to oxygenate the baby’s brain and vital organs. Not cutting the cord allowed the baby to receive the blood from the placenta and kept the baby’s blood pressure more stable. All babies should remain attached to their placentas, when ever possible, until they have made the transition to extrauterine life. They know when to stop using the placenta!
As midwives, we have been delaying cord clamping as a standard protocol for decades. I am so pleased to see the pendulum swinging so that we can save newborns born prematurely with the possibility of no neurological deficits.
Curious about lotus births…what is your experience and do you have references to support this practice? Thank you.
Hi Rainey Lotus Birth is available as an ebook and you can see http://www.lotusbirth.net