*This blog was previously published at www.summahealth.org
My name is Jennifer Doyle. As women’s health nurse practitioner and breast cancer survivor, I was asked to share excerpts from a 4-part blog that was published as part of my Health System’s ‘Flourish’ series in 2013. Only 5 days ago, I passed the ‘5 year mark’ from diagnosis. Thank you for allowing me to share my story, which I hope may help others who face breast cancer.
Diagnosis: “I am NOT a pink ribbon”
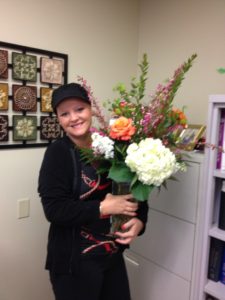 I was diagnosed with breast cancer on Sept. 24, 2012. I was not necessarily shocked, as all three of my father’s sisters had been diagnosed with breast cancer by the age of 50. I found a lump through a self-breast exam, and within a week had my diagnosis. I noticed the lump a few months prior, but it was very small and very hard. I figured it was just my monthly cycle. However, when I re-checked my breast in the shower, it was much, much larger and hard as a rock. I could not move it. I could not find the edges of the mass on palpation. When I got out of the shower and looked in the mirror, I saw the orange peel affect, or dimpling of the skin around the area, and instantly knew that I had breast cancer.
I was diagnosed with breast cancer on Sept. 24, 2012. I was not necessarily shocked, as all three of my father’s sisters had been diagnosed with breast cancer by the age of 50. I found a lump through a self-breast exam, and within a week had my diagnosis. I noticed the lump a few months prior, but it was very small and very hard. I figured it was just my monthly cycle. However, when I re-checked my breast in the shower, it was much, much larger and hard as a rock. I could not move it. I could not find the edges of the mass on palpation. When I got out of the shower and looked in the mirror, I saw the orange peel affect, or dimpling of the skin around the area, and instantly knew that I had breast cancer.
When it came to the actual diagnostic process, it was quite memorable. I recall going in for the mammogram, already believing in some part of my brain that I had breast cancer. I thought to myself, “Hey, if I get my mammogram and get out of here, I’m good. If they keep me for an ultrasound, I’m screwed.” I had the mammogram, and wouldn’t you know it, I needed to stay for an ultrasound. As I sat waiting for the ultrasound, and again waiting for the ultrasound results, I watched women come and go from the breast center. They came in talking on their phones, making lunch plans; in and out. I was jealous. I wanted to just get up and go on with my life, too. Yet, I already knew that I could not.
Then came the inevitable. I was taken into a room with a tech and a physician, and informed that I needed a biopsy – today if possible. I was told that I had a mass in my right breast and that it was “very suspicious.” When the staff members left the room, I sat somewhat stunned. I looked around and realized I was surrounded by pink ribbons. There were quilts and pictures all hailing the pink ribbon. I instantly hated the color pink. Everything in me rebelled against the pink ribbon. I thought, “I want nothing to do with any of this. I am NOT a pink ribbon. I will not be defined by this!”
My formal diagnosis came via a phone call from my OB/GYN. Despite being a Women’s Health Nurse Practitioner, I said “I work in OB; I don’t know anything about breast cancer! What does this mean?” He informed me that it was the most common type of breast cancer, invasive ductal carcinoma, and that he was referring me to a general surgeon. My path was laid out before me, and I began my journey….
Treatment-“Wow, you look like GI Jane!”

My husband, Tim was with me for the biopsy and the diagnosis. One of the most challenging days was the day I had to tell my parents and our 13-year-old daughter, Claire, Someone wisely told me that the most difficult part of dealing with cancer is dealing with others’ reactions and emotions. It is so true. I rarely worry, but I hate being the cause for worry in the people I love. What I would say about Claire and my recovery is simple: She was ALL of my reasons.
After I broke the news to my family, my Breast Care Coordinator Heidi Eve Cahoon, MSN, CNP, of Summa’s Jean and Milton Cooper Cancer Center in Akron, met with myself, my husband, and my parents. She explained the pathology report and typical course for the breast cancer patient. We all felt more informed and educated after meeting with her. If you’re coping with the same diagnosis, it’s worth reading more about how breast cancer navigators can help you through treatment.
I opted for chemotherapy prior to any surgery. This was due in part to medical recommendations, but it appealed to me because it bought me time to assess my options for surgery and/or radiation. My four rounds of chemotherapy included “AC,”which stands for Adriamycin and Cytotoxin (sounds so lovely). The very first round of chemo came with a side of the vomits. I began vomiting within four hours of leaving treatment, and this continued for a couple of days. Thankfully Dr. R. Douglas Trochelman (my oncologist) and the nurses changed up my antiemetic medications, and I did not experience any vomiting during the last three rounds.
Chemotherapy is quite interesting. The ‘chemical menopause’ ceased periods and brought on hot flashes. The nausea, the vomiting, mouth sores, and the utter exhaustion were novel and unwanted companions. Hair loss seemed to be the most focused-on side effect by nearly everyone. I followed the advice given to me: Buy a wig. Buy two wigs. Be prepared. I spent $400 on wigs. When the time came and the hair began to fall, my husband and I went into the bathroom. Clippers in hand, my remaining blonde locks fell all around. A tear or two did escape. But then my husband looked at me with wide eyes and said, “Wow, you look like GI Jane!” I regarded myself in the mirror for some time and decided I didn’t mind the bald chick look. I briefly tried wigs but found them intolerable. I decided to rock the new look and traded up the wigs for bandanas, ball caps, and very often, nothing at all!

I underwent a double mastectomy at Summa Health Akron in early February 2013. I chose to have this, despite being a “good candidate” for a lumpectomy. I did not have either of the BRCA genes. However, I wonder how many genes are there out there that we do not know about yet? Part of my reasoning was a desire to avoid radiation. The other was family history. My general surgeon performed the double mastectomy and my plastic surgeon placed tissue expanders. I took the Scarlett O’Hara approach to the double mastectomy. I did not think about it. I thought, “I will think about it when it is over.” I woke up after surgery and a funny thing happened. I actually was OK. I did not mourn my breasts. The pain was tolerable. I thought I was over halfway through my journey, when the road took an unexpected turn. My lymph nodes removed during surgery tested positive for cancer.
Somewhere in the back of my mind I heard a game show announcer: “Jennifer Doyle, guess what YOU’VE won?! Four more rounds of chemotherapy!” I endured four more rounds of chemotherapy with the drug Taxol. No nausea, vomiting, or mouth sores, but the exhaustion persisted, and I experienced exquisite bone pain.
Breast reconstruction following mastectomy is quite novel and interesting. There are many options, from flaps to implants to prosthetics. Would you like a nipple created? Did you keep your own? Or would you like a nipple tattooed on? I chose to go with implants. What I would choose for nipples; Stars? Flowers? This was one of amusing things I thought about while going through the process.
It wasn’t easy as it seemed. In order to get implants, one must first endure the tissue expanders. The tissue expanders are like balloons made of tire tread. They are placed during mastectomy. A series of injections expands the balloon. The skin expands and stretches, giving the plastic surgeon a pocket, or space to place the implant, and adequate skin to cover the new implant. I began going to my plastic surgeon’s office for weekly expansion. I referred to them as my “pump me up” sessions.
The first time the nurse came in with the two large 60 cc syringes and extra-long needles, my husband swore and exclaimed, “Are you going to hit her heart with that?!” This was the expansion process. For me, it was one of the most painful processes of breast cancer. My husband went with me to nearly every expansion. When he could not go, my parents went. I always had Tim or my mom there to hold my hand during the expansion. I know it sounds wimpy. But, hey, it helped!
As I waited for my final surgery, a combination of breast reconstruction and oophorectomy (ovary removal), life went on. I went back to work at Summa Health’s Women’s Health Services Department once chemo was over.
A Successful Journey: “There is a lesson in every joy and every sorrow.”

I believe three factors have made my journey a success, even though the ending yet eludes me, and the outcome is not set in stone. First, is the seemingly endless support I have received from my family and friends. The care and outpouring has been humbling and heartwarming, to say the least. I am glad it was me who has breast cancer, and not my mom or sisters, though I know they would trade places with me. You see, as a baby, I was born with multiple birth defects and spent a large part of my childhood sick, undergoing surgery, or admitted to the hospital. So for me, medical issues are nothing new. I’m not Superwoman. It’s just that I take such things in stride; that is the second factor. The third factor is faith. From the diagnosis until now, my faith has held fast. I have always believed that everything has purpose. If it were not for my childhood challenges, I probably would not have become a nurse. There is a lesson in every joy and every sorrow. It may sound hard to believe, but I have never asked God “Why?”I have also never asked God to cure me. I have simply prayed for two things:
One, that God grants me the strength to endure this with dignity and grace, no matter what, and two, “Thy will be done.”
On July 8, I underwent my final two surgeries. The surgeries included reconstruction and an oophorectomy (ovary removal). You may recall that my reconstruction choice was tissue expansion followed by silicone breast implants. Both surgeries went very well. I actually woke up feeling a bit more comfortable than I did going into surgery. The implants are much better than tissue expanders! I consider myself lucky to have had such a fabulous care team of Summa Akron City Hospital nurses and surgeons!
Survivorship
Fast forward five years. It is hard to believe all that has happened since Sept., 2012. Now it is Sept, 2017 and I am President-Elect of AWHONN! Claire is now a senior in high school and will leave for college next summer. I am grateful every day for the opportunity to contribute in a meaningful way both in my personal and professional life. For now, I have defeated cancer. However, cancer and I have each left our mark on the other. I still experience some discomfort most every day in my right chest and axillary region. Not exactly sure why that is, but it is most likely related to scarring and adhesions. I still cannot lift my right hand very far above my head unless manually assisted. Opening a can or bottle comes with significant difficulty that offers a regular reminder. I continue to experience aphasia from time to time; this peaked during chemotherapy and has not completely left. Finally, the neuropathy in my feet remains profound. I have very little feeling in my feet and most of the time; they just feel ‘asleep’. That can be really annoying, to say the least. Despite some of these physical effects, I am overall quite healthy and physically active.
 Once cancer has personally impacted your life, there may always be some small measure of worry in the deep (or not so deep) recesses of your brain. Cancer can become a lifelong resident in your mind: What if it comes back? Is that a lump or just scar tissue? I cannot believe that anyone is immune to these doubts that come to call on occasion. What I think is important is to own your thoughts and where you allow those thoughts to go. Of course I have fears, but I remind myself to center and to refocus my thoughts and efforts in another direction. Sometimes this takes specific intention. In every story, there is meaning. While I still have not fully come to understand the meaning of my breast cancer, perhaps it will be made clear to me one day. Lessons learned via a renewed appreciation for life’s small moments are perhaps what I take from this part of my journey. Every person has a unique story and must come to their own point of resolution and peace. I thank you for allowing me this opportunity to share some of my experiences.
Once cancer has personally impacted your life, there may always be some small measure of worry in the deep (or not so deep) recesses of your brain. Cancer can become a lifelong resident in your mind: What if it comes back? Is that a lump or just scar tissue? I cannot believe that anyone is immune to these doubts that come to call on occasion. What I think is important is to own your thoughts and where you allow those thoughts to go. Of course I have fears, but I remind myself to center and to refocus my thoughts and efforts in another direction. Sometimes this takes specific intention. In every story, there is meaning. While I still have not fully come to understand the meaning of my breast cancer, perhaps it will be made clear to me one day. Lessons learned via a renewed appreciation for life’s small moments are perhaps what I take from this part of my journey. Every person has a unique story and must come to their own point of resolution and peace. I thank you for allowing me this opportunity to share some of my experiences.
My life was certainly entangled in the pink ribbon for some time. Now, that has come full circle. Today I embrace that ribbon and am proud to wear it as a banner symbolizing survival.
 Jennifer Doyle is a WHNP with nearly 25 years of experience in obstetrics. She is the APN of the Women’s Service Line at Summa Health in Akron, Ohio as well as Faculty and Coordinator of the WHNP program at Kent State University in Kent, OH. She is AWHONN’s President elect in 2017 and is happy to share her personal story from the perspective of a breast cancer patient.
Jennifer Doyle is a WHNP with nearly 25 years of experience in obstetrics. She is the APN of the Women’s Service Line at Summa Health in Akron, Ohio as well as Faculty and Coordinator of the WHNP program at Kent State University in Kent, OH. She is AWHONN’s President elect in 2017 and is happy to share her personal story from the perspective of a breast cancer patient.
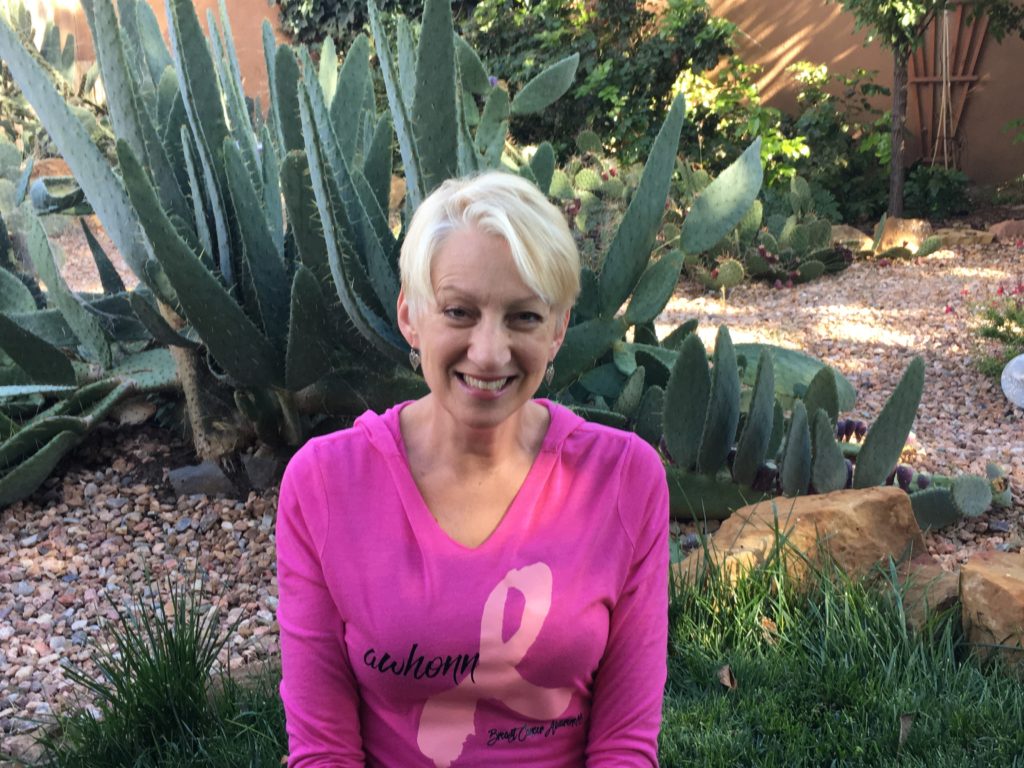







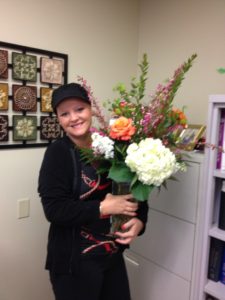 I was diagnosed with breast cancer on Sept. 24, 2012. I was not necessarily shocked, as all three of my father’s sisters had been diagnosed with breast cancer by the age of 50. I found a lump through a self-breast exam, and within a week had my diagnosis. I noticed the lump a few months prior, but it was very small and very hard. I figured it was just my monthly cycle. However, when I re-checked my breast in the shower, it was much, much larger and hard as a rock. I could not move it. I could not find the edges of the mass on palpation. When I got out of the shower and looked in the mirror, I saw the orange peel affect, or dimpling of the skin around the area, and instantly knew that I had breast cancer.
I was diagnosed with breast cancer on Sept. 24, 2012. I was not necessarily shocked, as all three of my father’s sisters had been diagnosed with breast cancer by the age of 50. I found a lump through a self-breast exam, and within a week had my diagnosis. I noticed the lump a few months prior, but it was very small and very hard. I figured it was just my monthly cycle. However, when I re-checked my breast in the shower, it was much, much larger and hard as a rock. I could not move it. I could not find the edges of the mass on palpation. When I got out of the shower and looked in the mirror, I saw the orange peel affect, or dimpling of the skin around the area, and instantly knew that I had breast cancer.


 Once cancer has personally impacted your life, there may always be some small measure of worry in the deep (or not so deep) recesses of your brain. Cancer can become a lifelong resident in your mind: What if it comes back? Is that a lump or just scar tissue? I cannot believe that anyone is immune to these doubts that come to call on occasion. What I think is important is to own your thoughts and where you allow those thoughts to go. Of course I have fears, but I remind myself to center and to refocus my thoughts and efforts in another direction. Sometimes this takes specific intention. In every story, there is meaning. While I still have not fully come to understand the meaning of my breast cancer, perhaps it will be made clear to me one day. Lessons learned via a renewed appreciation for life’s small moments are perhaps what I take from this part of my journey. Every person has a unique story and must come to their own point of resolution and peace. I thank you for allowing me this opportunity to share some of my experiences.
Once cancer has personally impacted your life, there may always be some small measure of worry in the deep (or not so deep) recesses of your brain. Cancer can become a lifelong resident in your mind: What if it comes back? Is that a lump or just scar tissue? I cannot believe that anyone is immune to these doubts that come to call on occasion. What I think is important is to own your thoughts and where you allow those thoughts to go. Of course I have fears, but I remind myself to center and to refocus my thoughts and efforts in another direction. Sometimes this takes specific intention. In every story, there is meaning. While I still have not fully come to understand the meaning of my breast cancer, perhaps it will be made clear to me one day. Lessons learned via a renewed appreciation for life’s small moments are perhaps what I take from this part of my journey. Every person has a unique story and must come to their own point of resolution and peace. I thank you for allowing me this opportunity to share some of my experiences. Jennifer Doyle is a WHNP with nearly 25 years of experience in obstetrics. She is the APN of the Women’s Service Line at Summa Health in Akron, Ohio as well as Faculty and Coordinator of the WHNP program at Kent State University in Kent, OH. She is AWHONN’s President elect in 2017 and is happy to share her personal story from the perspective of a breast cancer patient.
Jennifer Doyle is a WHNP with nearly 25 years of experience in obstetrics. She is the APN of the Women’s Service Line at Summa Health in Akron, Ohio as well as Faculty and Coordinator of the WHNP program at Kent State University in Kent, OH. She is AWHONN’s President elect in 2017 and is happy to share her personal story from the perspective of a breast cancer patient.

 Shelley Thibeau, PhD, RNC, is the Director of the developing Mothers’ Milk Bank of Louisiana. As a NICU nurse for 38 years, her interest in breastmilk has expanded to exploring breastmilk immunology associated with preterm infant health.
Shelley Thibeau, PhD, RNC, is the Director of the developing Mothers’ Milk Bank of Louisiana. As a NICU nurse for 38 years, her interest in breastmilk has expanded to exploring breastmilk immunology associated with preterm infant health.
 Tasha Poslaniec has been a registered nurse for 17 years. She has been working in obstetrics for over a decade and is currently a Perinatal Quality Review Nurse and Childbirth Educator.
Tasha Poslaniec has been a registered nurse for 17 years. She has been working in obstetrics for over a decade and is currently a Perinatal Quality Review Nurse and Childbirth Educator.
 Deirdre Wilson, Senior Editor for UbiCare, is an award-winning writer and editor with 30 years’ experience researching and writing on a wide range of health, wellness and education topics for newspapers, magazines and a news wire service.
Deirdre Wilson, Senior Editor for UbiCare, is an award-winning writer and editor with 30 years’ experience researching and writing on a wide range of health, wellness and education topics for newspapers, magazines and a news wire service.
 Kate McNair is a women’s health nurse practitioner & PhD student at Boston College. She also maintains clinical practice as an OB/GYN RN at a community health center in Roxbury, MA. Follow her on Twitter
Kate McNair is a women’s health nurse practitioner & PhD student at Boston College. She also maintains clinical practice as an OB/GYN RN at a community health center in Roxbury, MA. Follow her on Twitter 
 Lynn Erdman, MN, RN, FAAN,
Lynn Erdman, MN, RN, FAAN,