 by, Kathleen Tavenner Mitchell, MHS, LCADC
by, Kathleen Tavenner Mitchell, MHS, LCADC
“Your daughter has full-blown fetal alcohol syndrome.”
Those words hit me like a tsunami. I was drowning in waves of grief, disbelief, horror and remorse. For 15 years, I searched to understand why Karli wasn’t learning and growing stronger, like my other two children. Doctors told me ear infections had caused her minor delays, but she would “grow out of it.” Today, Karli is 42 years old; developmentally, she is about 6 years old.
I grew up in the 1960s in an upper middle-class suburban neighborhood. My charismatic father suffered with alcoholism, and my co-dependent mom worked hard to cover his tracks. At 16, I was already experimenting with alcohol and other drugs when I got pregnant, married and dropped out of school. I wanted to have a healthy baby so I gave up all of the drugs and drank apple wine on the weekends.
 Effects of Alcohol in Pregnancy
Effects of Alcohol in Pregnancy
My first child, a boy, was born with a clubbed foot, which the doctor told me was a genetic disorder. I had Karli a year later, when the research describing fetal alcohol syndrome (FAS) was published. A few years later, I gave birth to another daughter and still had never been told not to drink during pregnancy.
I divorced my high school sweetheart and remarried another man who liked to drink. My own issues with alcoholism and addiction spiraled out of control. I had two unplanned pregnancies while on methadone to treat my heroin addiction. No one at the clinic ever mentioned that it wasn’t OK to drink. My second son came prematurely and died the day he was born. After a full-term pregnancy with my third baby girl, I found her breathless in her crib at 10 weeks old: Sudden Infant Death Syndrome (SIDS). I didn’t realize how those years of addiction affected each of my children.
No Safe Amount of Alcohol
Fetal alcohol spectrum disorders (FASDs) are a group of conditions that can occur in a person whose mother drank alcohol during pregnancy. Most people with FASD don’t have intellectual disabilities, but do have attention deficits, behavioral issues, learning disabilities, mental health issues, and problems with memory, judgment and reason. Each person can be affected in different ways and, often, a person with an FASD has a mix of these problems. FAS is the most severe form of FASD.
Alcohol is a leading cause of fetal brain damage, birth defects and both fetal and infant death, including SIDS. While pregnant, there is no safe amount of alcohol, no safe time to drink alcohol, and no safe type of alcohol.
Clean and sober for the last 31 years, I have dedicated my life’s work to increasing awareness and improving services for individuals with FASD and for women dealing with addiction issues. I have a beautiful marriage and 5 wonderful grandchildren. I went on to receive my Master of Human Services (MHS) degree and became a licensed clinical alcohol and drug counselor (LCADC). I know that treatment works, and by encouraging women to get help, we save their children too. Now I am that good mother I always wanted to be.
If you’re struggling or think your child may be affected by FASD, don’t hesitate to reach out to your nurse, midwife or other healthcare provider. There is no shame in asking for help—your child’s life depends on it.
Fetal Alcohol Syndrome Disorder (FASD)
- FASD’s effects are lifelong—but they’re also preventable
- Alcohol in pregnancy is more harmful than any other recreational drug, including cocaine, heroin and marijuana
- Alcohol can damage a developing baby before you even know you’re pregnant
- FASD is rarely diagnosed, making it an invisible disorder
Source: NOFAS.org
 Kathleen is vice president of the National Organization on Fetal Alcohol Syndrome (NOFAS).
Kathleen is vice president of the National Organization on Fetal Alcohol Syndrome (NOFAS).
Resources
- Get Help: Circle of Hope
- Learn More: http://www.health4mom.org/alcohol_in_pregnancy_how_much_is_safe
FASD PREVENTION PROJECT
AWHONN is a national partner on the Fetal Alcohol Spectrum Disorders Prevention Project of the Arc, a non-profit advocacy organization serving people with intellectual and developmental disabilities. The goal of the FASD Prevention Project is to increase health care professional knowledge of the risks alcohol can pose to a fetus, encourage the use of FASD prevention strategies and provide educational opportunities to health care professionals, including nurses, midwives, and nurse practitioners. Learn more about this project and resources you can use.



 Danni Starr
Danni Starr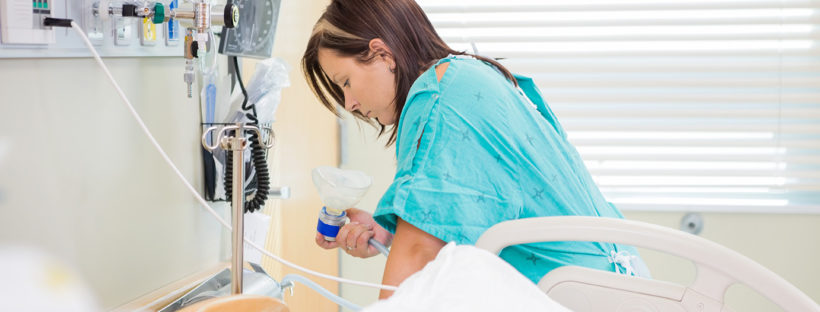

 Michelle Collins is currently Professor of Nursing and Director of the Nurse-Midwifery education program at Vanderbilt University School of Nursing. In addition to the teaching and administrative aspects of her job, she maintains an active clinical practice as part of the Vanderbilt School of Nursing faculty nurse-midwifery practice. Currently she is a blogger for Nashville Public Television for the popular series Call the Midwife.
Michelle Collins is currently Professor of Nursing and Director of the Nurse-Midwifery education program at Vanderbilt University School of Nursing. In addition to the teaching and administrative aspects of her job, she maintains an active clinical practice as part of the Vanderbilt School of Nursing faculty nurse-midwifery practice. Currently she is a blogger for Nashville Public Television for the popular series Call the Midwife.

 Jessica L. Grenon is the Director of Continuing Education Services at The Conference Exchange, where she has worked with AWHONN since 2007. She, her husband, and their two young children enjoy traveling and spending time with their extended family, especially with her twelve nieces and nephews.
Jessica L. Grenon is the Director of Continuing Education Services at The Conference Exchange, where she has worked with AWHONN since 2007. She, her husband, and their two young children enjoy traveling and spending time with their extended family, especially with her twelve nieces and nephews.






 Aimee Poe is an experience specialist at Verizon. She loves playing video games, watching movies, hanging out with her family, and flexing her creative muscle with various projects.
Aimee Poe is an experience specialist at Verizon. She loves playing video games, watching movies, hanging out with her family, and flexing her creative muscle with various projects.



